Struggling with shooting leg pain, numbness, or weakness?
Quick Answer: Sciatica is nerve pain caused by irritation or compression of the sciatic nerve — most commonly from a lumbar disc bulge. Evidence-based physiotherapy is the recommended first-line treatment, and most people improve significantly within 6–12 weeks without surgery.
What Is Sciatica? (And What Most People Get Wrong)
Sciatica isn’t a diagnosis — it’s a symptom pattern.
It describes pain, numbness, tingling, or weakness that travels from the lower back or buttock down the back of the thigh and leg — sometimes into the foot. The pain follows the path of the sciatic nerve, which forms from nerve roots at L4–S1 in the lower spine.
The key question is: what’s irritating the nerve?
At AlphaCare Physiotherapy in Mitchell Park, we identify the exact source of nerve irritation because treatment differs depending on the cause.
What Does Sciatica Actually Feel Like?
- Burning or electric shock–like pain shooting down one leg
- Deep buttock ache worse after 10–15 minutes of sitting
- Pins and needles in the calf or foot
- Leg weakness (difficulty pushing off when walking)
- Morning stiffness or pain after rest
- Relief with gentle walking but worse with bending or lifting
Sciatica usually affects one side. If symptoms occur in both legs, or you notice bladder/bowel changes or groin numbness, seek urgent medical care.
The 4 Most Common Causes of Sciatica
1. Lumbar Disc Bulge or Herniation (Most Common)
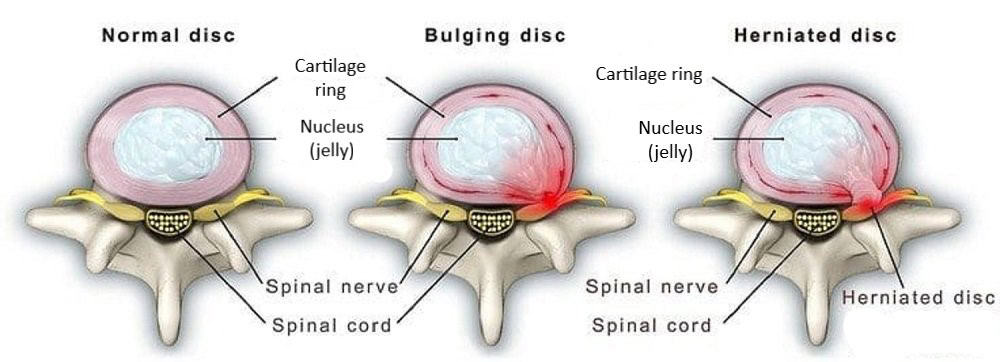
The intervertebral discs act as shock absorbers. When a disc bulges (commonly at L4/L5 or L5/S1), it can compress the exiting nerve root.
- Worse with sitting or bending
- Pain with coughing or sneezing
- Often affects people aged 30–55
2. Piriformis Syndrome (Deep Gluteal Syndrome)
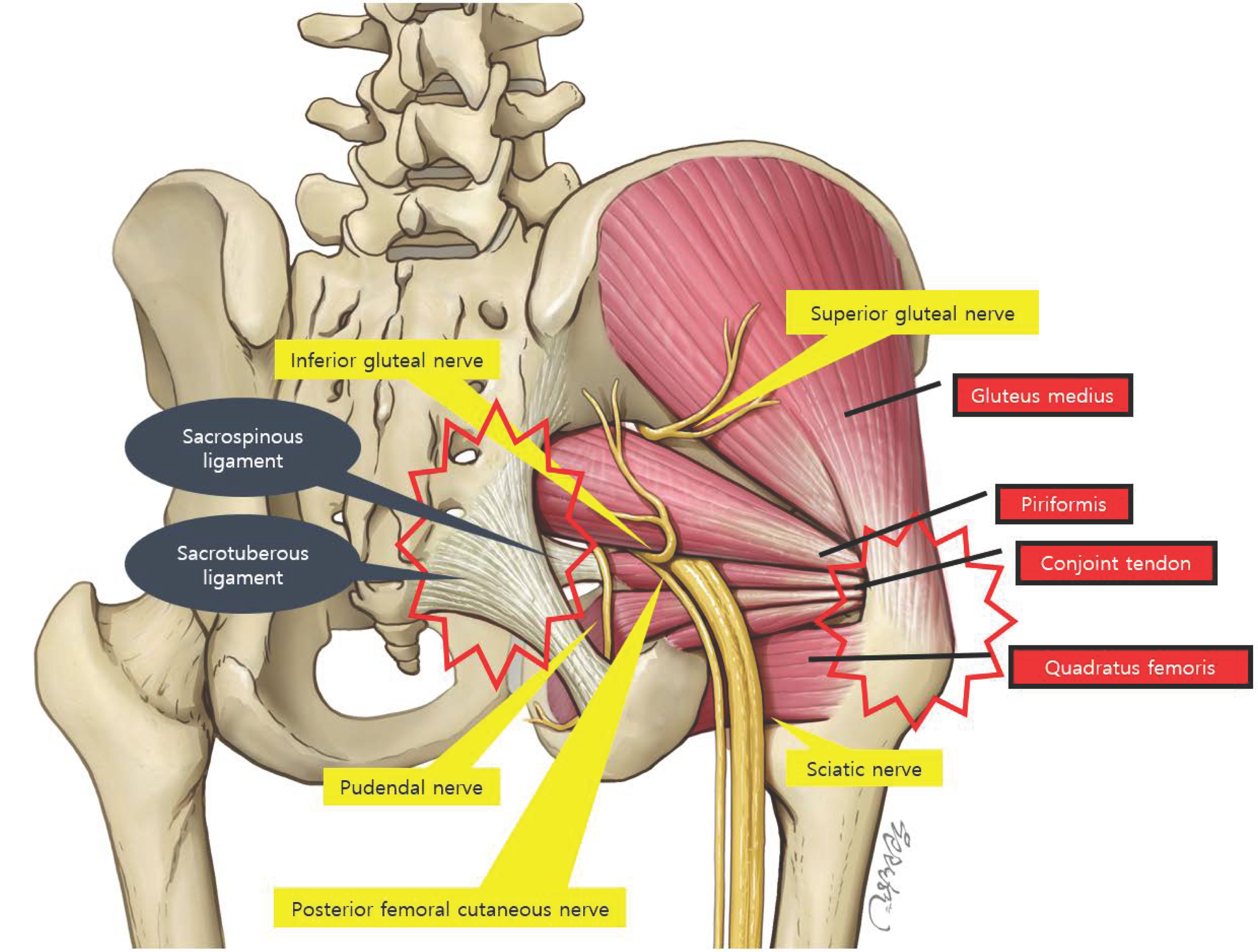
The sciatic nerve passes beneath (and sometimes through) the piriformis muscle. Tightness or inflammation here can compress the nerve.
- Deep buttock tenderness
- Worse going from sitting to standing
- Often linked to prolonged sitting or running
3. Lumbar Spinal Stenosis
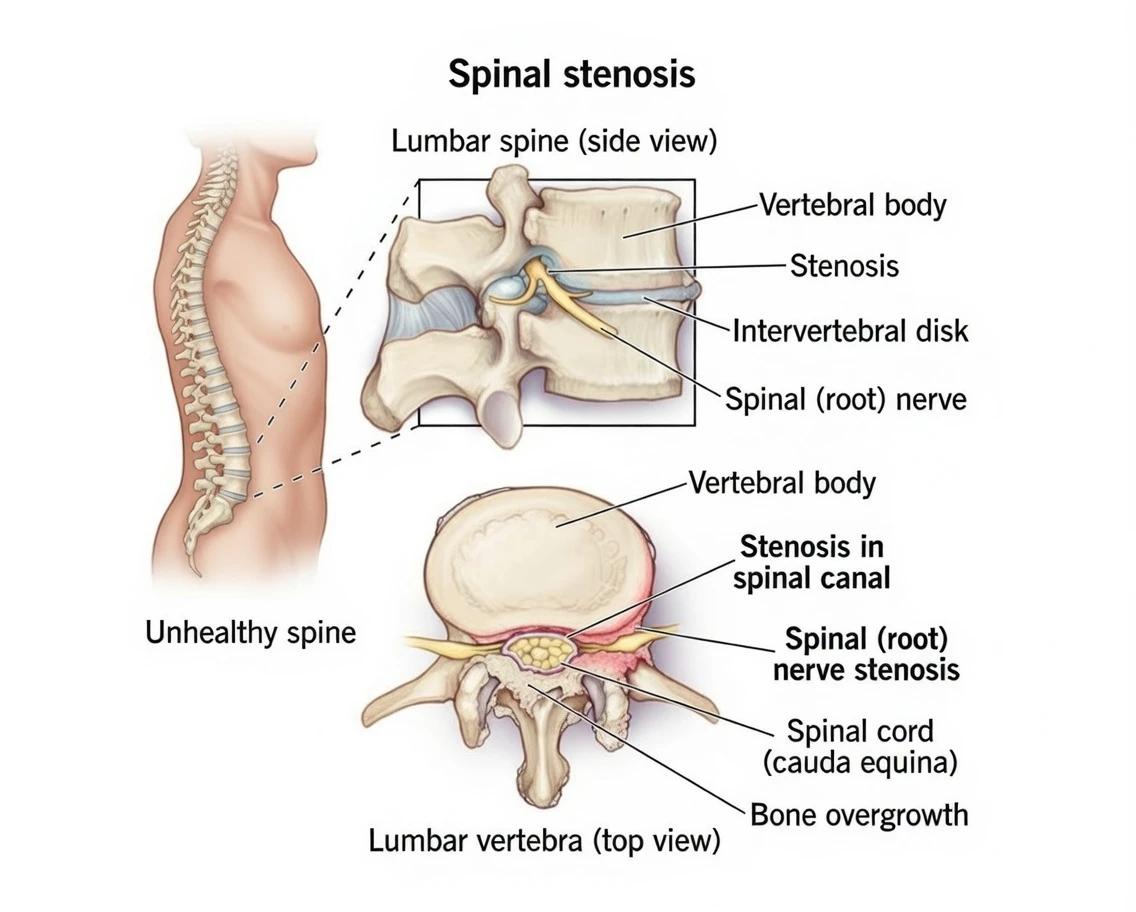
Age-related narrowing of the spinal canal can compress nerve roots.
- Worse with walking or standing
- Relief when sitting or leaning forward
- More common over age 60
4. Spondylolisthesis
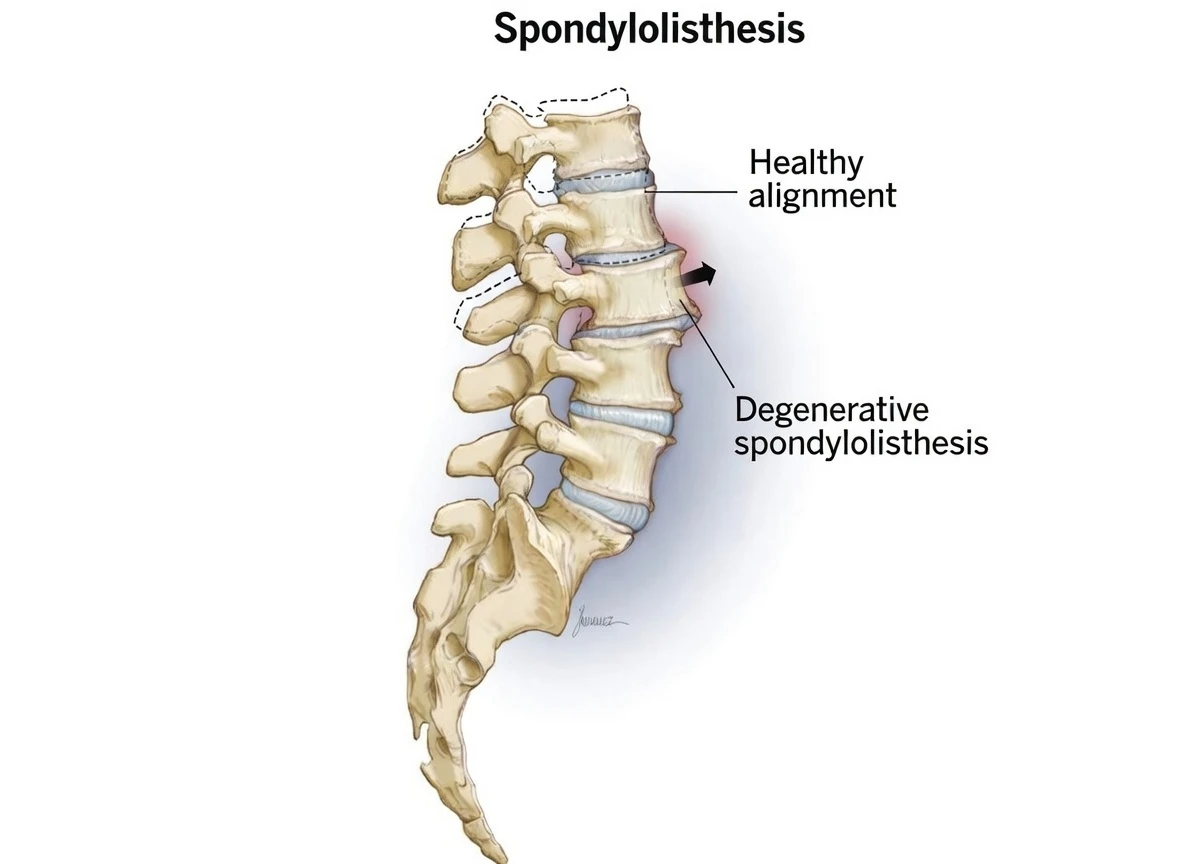
One vertebra slips forward over the one below it, irritating nearby nerves.
- Long-standing back pain history
- Gradual development of leg symptoms
Does Sciatica Go Away on Its Own?
- ~90% improve within 6–12 weeks
- Bed rest does not improve outcomes
- Staying active improves recovery
- Physiotherapy reduces recurrence risk
How We Assess Sciatica
- Detailed history
- Neural testing (SLR, Slump)
- Spinal movement assessment
- Strength and sensation testing
- Postural analysis
What Actually Works
- Manual therapy
- Neural mobilisation
- Targeted strengthening
- Ergonomic advice
- Education and load management
Do You Need an MRI?
Usually no. Imaging is considered if progressive weakness, severe neurological deficit, or no improvement after 6–8 weeks.
